
[cmamad id=”20916″ align=”center” tabid=”display-desktop” mobid=”display-desktop” stg=””]
New scientific data shows that Big Pharma and the FDA have been lying about heart disease… It turns out cholesterol and saturated fats are not to blame…
—-Important Message—-
Is Big Pharma Working With the FDA to Cover up This Cancer Cure?
Have you ever heard of GcMAF?
Scientific data shows that GcMAF can cure cancer naturally, making Big Pharma treatments obsolete…
But every lab that tries to study GcMAF gets raided and shut down by the FDA…
And every health researcher who tries to go public with this natural cure dies or disappears…
I have a feeling something funny is going on… So I started looking for the GcMAF research that Big Pharma tried to bury…
Here’s everything I could dig up about this natural cancer cure, GcMAF…
————
They’re Lying About Heart Disease – Here’s Why
The supposed “risk factors” of cardiovascular disease (CVD) are cholesterol, low-density lipoprotein, and saturated fatty acids.
These notions are all grounded in antiquated 1950s science.
This view was a bastardization of science, a charade, a gross simplification that was fed to the public by the AMA (American Medical Association)…
And it was further distorted by the food industry…
But it is still defended because of a reluctance to admit error.
However, we have now over a century’s worth of newer scientific data to draw upon.
And I can see no reason to continue caving in to such an obviously incorrect party line.
Science has now made it possible for a more refined understanding of CVD – based on ascorbate and unsaturated fatty acids.
During the early era of Ancel Keys (the American physiologist who came up with the modern diet/heart hypothesis), so many things were not known yet…
Molecules such as thromboxane A2, selenocysteine, and apoprotein(a) hadn’t even been discovered then.
They didn’t even make a distinction between the two linolenic acid isomers, alpha and gamma.
Although very similar chemically, there is a world of difference between the two biologically.
The first dietary “risk factor” to gain widespread traction was cholesterol.
That was because cholesterol ingression is a very common postmortem finding in people with cardiovascular disease – so they still assumed it was the cause.
But it became clear that eating cholesterol does little to raise serum cholesterol (because you just synthesize less of it yourself)…
So epidemiologists inducted saturated fatty acids into the club of dietary “risk factors.”
“It is now clear that dietary cholesterol per se, which is contained in almost all foods of animal origin, has little or no effect on the serum cholesterol concentration in man.” ―Ancel Keys, 1956
[cmamad id=”20917″ align=”center” tabid=”display-desktop” mobid=”display-desktop” stg=””]
This is because eating long-chained saturated fatty acids actually slightly increases circulating cholesterol, a steroid that supposedly then “deposits itself on the arterial wall.”
Yet saturated fats don’t increase the synthesis of cholesterol any more than glucose does.
It merely causes its redistribution into the blood.
Saturated fatty acids go through the portal vein towards the liver and then are packaged, along with cholesterol, inside lipoproteins.
However, unsaturated fatty acids tend more to form chylomicrons, which are absorbed into the body more quickly.
Unsaturated fatty acids will do this because of their relatively bent lipid chains and their double bonds, making them more permeable through the intestinal wall.
The aftershocks of this overly simplistic cholesterol model resound to this day…
And the phrase “saturated fat and cholesterol” has become a cliché.
This hypothesis was solidified back in the day by Ancel Keys’ “Seven Countries Study.”
That study compared dietary intakes against the presence of CVD disease in Yugoslavia (Serbia, Dalmatia, and Slavonia), Finland, Greece (Crete and Corfu), Italy, Japan, the Netherlands, and the United States.
But using these particular countries actually hid the true contribution of omega-6 fatty acids…
By lumping omega-6 (seed oils) in with omega-3 (marine oils) under the same “polyunsaturated” heading, the causative nature of omega-6 was obscured by the counteractive effect of omega-3.
Omega-6 fatty acids induce CVD disease in two ways:
1) They can form thromboxane A2, a powerful platelet-aggregating prostaglandin that causes thrombosis.
2) They can displace DHA from the cell membrane thereby promoting cholesterol ingression.
On the other hand:
1) Omega-3 fatty acids elongate into eicosapentaenoic acid, which goes on to form the blood-thinning thromboxane A3
2) DHA occupies the cell membrane and powerfully repels cholesterol while enhancing glucose flux.
The high omega-3 populations in Keys’ study (Japan, Italy, Greece) effectively offset the high omega-6 populations (e.g. Slavonia, Finland, Serbia).
A statistician who doesn’t differentiate between the two subtypes of polyunsaturated fatty acids (PUFAs) – omega-6 and omega-3 – will naturally see a low correlation (if any) between cardiovascular disease and PUFAs as a general class.
So the results of such a study would depend on what countries are chosen.
In fact, Japan and Greece actually have the highest omega-3 to omega-6 intake ratio.
So, of course, that would obscure the role of PUFAs in the “Seven Countries Study.”
The chart below shows the omega-6 to omega-3 ratios of several populations.
You can see the ratio was very low in caveman days and it’s low in Greece and Japan.
But it’s very high in the US and in urban India.
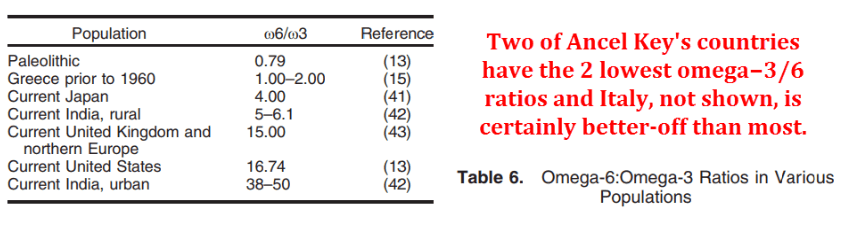

If Keys had discriminated between the two important types of PUFAs, and if he had included India, he would never have come to the “saturated fats and cholesterol” conclusion.
The correlation against omega-6 fatty acids is so strong that it can’t be denied…
That risk factor implies that urban India would be the world’s epicenter for CVD because they consume the highest omega-6/3 ratio.
This presents a dilemma for the “Keys Club” – urban Indians are mostly vegetarian and consume very little cholesterol.
So, according to that doctrine, the Indian population should be at very low risk for CVD.

Indians also eat relatively small amounts of saturated fats (many do eat ghee, but it’s not a huge contribution to their diet).
So that should also put them at low risk for CVD.

But India is a world leader in CVD, with more deaths under the age of 60 than the US.
This is despite their vegetarianism, negligible cholesterol consumption, and relatively low intake of saturated fats.
“The Indian subcontinent (including India, Pakistan, Bangladesh, Sri Lanka, and Nepal) has among the highest rates of cardiovascular disease (CVD) globally.”
Since Indians consume negligible amounts of cholesterol, the naïve epidemiologists had to propose a litany of other risk factors to account for their high CVD rates.
Since they could not explain India’s high rate of CVD by salt, cholesterol, or saturated fatty acids…
…they simply waved a magic wand and pulled a motley array of flaky risk factors out of a hat.
They used tobacco, alcohol, starch, trans-fatty acids, physical inactivity, urbanization, psychosocial factors, and cooked vegetables to explain the very high CVD rates in India.
Although smoking destroys vitamin C in the plasma, and cooking destroys some nutrients in foods, none of the other purported “risk factors” are very significant.
They even felt the need to reverse the protective role of alcohol when fumbling to explain India’s CVD rates.
“Although vegetarian, the meals of many South Asians consist of large quantities of carbohydrates such as rice and bread (which predisposes to atherogenic dyslipidemia including hypertriglyceridemia and low HDL cholesterol)…”
“ Moreover, the vegetables that are consumed are often overcooked (a process which has been shown to diminish their content of potentially protective micronutrients compared with raw or properly cooked vegetables.”
You don’t see a single peep there about omega-6 fatty acids…
And those supposed “risk factors” do not have very convincing biochemical mechanisms to cause CVD either…
…not compared to the straightforward and well-supported data implicating omega-6 fats and ascorbate.
About ascorbate (vitamin C)…
We need ascorbate to synthesize collagen, a strong structural protein that makes up a large part of the vascular wall.
For example, when someone has subclinical scurvy a low collagen turnover degrades the arterial wall.
In anticipation of this process, the body synthesizes apoprotein(a).
That is a protein similar to fibrin – with “lysine kringles” – that has an affinity for frayed collagen strands.
Apoprotein(a) is a subgroup of atoms of the larger lipoprotein(a), a circulating lipoprotein that carries cholesterol.
“It is…no surprise that lipoprotein(a), a combination of the adhesive protein apoprotein(a) with a low-density lipoprotein particle, became the most frequent genetic feature counteracting ascorbate deficiency.”
Lipoprotein(a) appears to be an evolutionary adaptation whereby our vessel walls are coated to keep us from bleeding out during times of low vitamin C intake.
The only animals that synthesize apoprotein(a) are the ones that cannot synthesize their own vitamin C.
And that is probably one reason why most animals make for poor models of human cardiovascular disease in the lab.
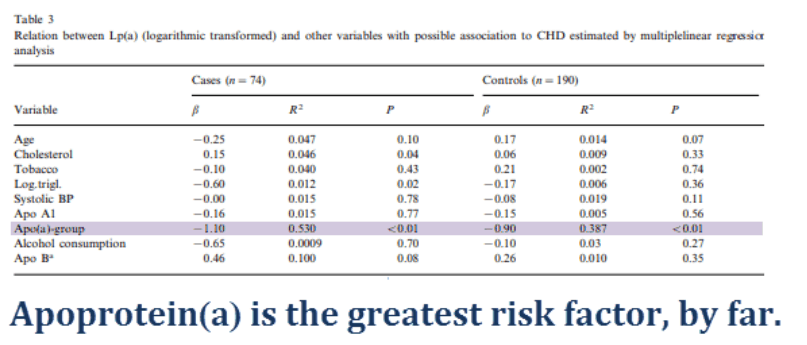
It may be worth noting that lipoprotein(a) – and/or its constituent apoprotein(a) – is the one blood factor most highly correlated with cardiovascular disease.
Omega-6 fatty acids tend to cause ischemic heart disease of a different sort, such as heart attack and stroke.
They do this by becoming thromboxane A2.
Thromboxane A2 is a powerful platelet-aggregating agent (technically a prostaglandin).
And this is why aspirin lowers the risk of ischemic heart disease.
The omega-3 analog, thromboxane A3, actually counteracts the pro-thrombotic action of thromboxane A2.
This is why the Inuit in Greenland have bleeding issues double that of their Danish neighbors – a population whose fat consumption is practically all omega-3 marine oils.
Other epidemiological evidence completely exonerates saturated fatty acids…
The traditional Polynesians of Tokelau consumed about 60% of their calories via coconuts with essentially no cardiovascular disease – yet the fat in coconuts is fully saturated.
Many other researchers have also noted the lack of correlation between heart disease and the classic “risk factors.”
Yet we keep hearing the same old annoying mantra over and over again in 2018 that “saturated fat and cholesterol cause cardiovascular disease.”
“Myocardial infarction commonly occurs in patients with none of the major known risk factors for the disorder. This suggests that important risk factors remain to be discovered.”
No matter how much statistical juggling the die-hard epidemiologists keep doing do to save the theory, the “saturated fat and cholesterol” theory simply does not fit.
And what doesn’t fit you must acquit.
Nothing seems to explain the two main forms of cardiovascular disease better than ascorbate and PUFAs.
Generations of us have grown up with these rules…
Shake these old wrong rules out of your head:
- Use margarine instead of butter (wrong)
- Use vegetable oils for salads and cooking (wrong)
- Don’t indulge in eggs (wrong)
Shove these rules into your head:
- Eat eggs – especially the yummiest part, the yolk!
- Make sure you eat lots of things full of vitamin C
- Use butter, coconut oil, and olive
Just keep in mind that it’s not good to have too much of ANY kind of fat, even if it’s a healthy fat.
—-Important Message—-
Quiz: Spot the diabetic-causing food that the US government recommends…

Think you know which food causes diabetes? Find out if you are right
————

- Cressman, Michael. "Lipoprotein (a) is an independent risk factor for cardiovascular disease in hemodialysis patients." Circulation (1992)
https://pdfs.semanticscholar.org/700d/9f512f7227d8702a36fa5e62461fe5dba997.pdf - Goyal, Abhinav. "The burden of cardiovascular disease in the Indian subcontinent." Indian Journal of Medical Research (2006)
https://pdfs.semanticscholar.org/5948/7de5d7c01948764ed807a59ee719f6be4458.pdf - Simopoulos, Artemis. "The importance of the omega-6/omega-3 fatty acid ratio in cardiovascular disease and other chronic diseases." Experimental biology and medicine (2008)
http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.559.7506&rep=rep1&type=pdf - Pauling, Linus. "A unified theory of human cardiovascular disease leading the way to the abolition of this disease as a cause for human mortality." Journal of Orthomolecular Medicine (1992)
http://momgil.cafe24.com/wp-content/uploads/2010/03/UnifiedTheory1.pdf - Phillips, Gerald. "Evidence for hyperestrogenemia as a risk factor for myocardial infarction in men." The Lancet (1976)
http://sciencedirect.com/science/article/pii/S0140673676929688
- Heart Disease Facts & Statistics | cdc.gov
https://www.cdc.gov/heartdisease/facts.htm - Heart Disease - Harvard Health
https://www.health.harvard.edu/topics/heart-disease-overview

Leave a Reply