
There are two basic requirements for getting diabetes.
And I’m talking about Type 2 diabetes.
Type 2 Diabetes is the most common kind — it’s often called adult onset diabetes.
This update will be our guide since it contains some of the latest research into what really causes diabetes.
 As the authors say, the two requirements for getting diabetes are insulin resistance, and a breakdown of the beta cells in the pancreas that produce insulin.
As the authors say, the two requirements for getting diabetes are insulin resistance, and a breakdown of the beta cells in the pancreas that produce insulin.
These two requirements shift the thinking on how diabetes develops.
This study shows that the old model of diabetes is wrong.
It used to be thought that diabetes was caused by continued insulin resistance.
By eating too much sugar and carbohydrates, you require your liver to produce a huge amount of insulin all the time.
High sugar and high carbohydrate foods are thought to cause so much insulin production, that eventually the cells stop listening to the insulin.
They become insulin resistant.
However this is not correct. It is completely wrong.
In fact, in another newsletter recently, I showed you a study showing that high sugar consumption correlates with a lower chance of getting diabetes.
And this is very important as we will see.
So one requirement to develop Type 2 diabetes is insulin resistance.
And the other requirement is a breakdown of the beta cells producing insulin.
So how do we get insulin resistance in the first place?
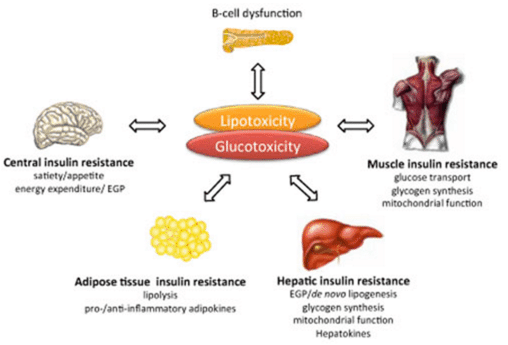 Insulin resistance takes place in the muscles and the liver, and even in the brain.
Insulin resistance takes place in the muscles and the liver, and even in the brain.
The biggest promoter of insulin resistance our free fatty acids in the blood.
In fact, as this paper shows us, even healthy people become insulin resistant when they are given free fatty acids via intravenous feeding.
And shockingly, it only takes a few hours for the change to happen.
Healthy people bounce back, and usually don’t remain insulin resistant.
But if they have a diet that is high in fat, especially PUFAs, they may continue to be insulin resistant.
Excessive dietary free fatty acid supply emerges due to induction of oxidative stress, by uncoupling oxidative phosphorylation but also by decreasing antioxidant defence mechanisms.
What the study is saying is this.
Eating a high-fat diet causes high levels of free fatty acids in the blood.
High free fatty acids levels stop the most efficient production of energy, called oxidative phosphorylation.
And high fats require significant antioxidant defense mechanisms.
This is especially true with PUFAs.
PUFAs require a great deal of antioxidant activity to neutralize them.
They are very toxic to the body.
And I believe they are the prime contributor to diabetes — especially to the diabetes epidemic that we’re going through right now.
Chronically high cortisol levels also cause insulin resistance.
In this paper they analyze the relationship between high cortisol levels and insulin resistance.
 Basically, cortisol causes the body to begin digesting its own tissues.
Basically, cortisol causes the body to begin digesting its own tissues.
This is a process known as gluconeogenesis.
In the long-term, higher cortisol results in shrinkage of the body.
This shrinkage is something that is often associated with being older, but also with being sicker.
And for promoting diabetes, high cortisol does one thing extremely well.
High cortisol increases free fatty acids, which cause insulin resistance.
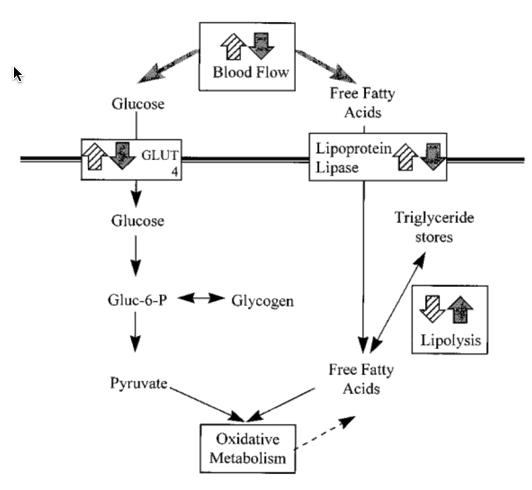 So now we know how we get insulin resistance.
So now we know how we get insulin resistance.
We have high cortisol levels, high levels of free fatty acids in our blood, and this makes is insulin resistant.
Now, what about the destruction of the beta cells that produce insulin?
As the first paper notes,
many obese patients do not develop T2DM although being severely insulin resistant.
To get diabetes, you need both insulin resistance and the destruction or neutralization of the beta cells that produce insulin.
You need both.
And I believe that what causes the destruction or neutralization of the beta cells is what this papers states.
Beta cell inflammation results from the whole body “internal inflammation”.
A large-scale internal inflammation process is seen in all type II diabetics.
All diabetics always have internal inflammation.
This can be identified through a test of C-reactive protein, the C-RP test or HS-CRP test.
And it’s another thing that can be identified by a chronically elevated cortisol level.
The cortisol is a reaction to inflammation.
The body pumps out more cortisol when it encounters more inflammation.
And what causes inflammation that causes diabetes?
I believe the entire answer lays in PUFAs.
PUFAs in our diet create large-scale destruction of our cells.
They cause chronic inflammation.
And eventually in many of us, PUFAs cause the destruction or neutralization of the insulin-producing beta cells in our pancreas.
What should you do now?
If you think you’re diabetic, or you are prediabetic, you may want to change your diet to minimize PUFAs.
You may want to minimize fats of all kinds.
And you may want to fix whatever it is that’s causing inflammation in your body.
If you have high blood pressure, if you have prostate inflammation, if you’re fat — then these are clues that you are suffering from internal inflammation.
And this raises the chances that you will become diabetic.
How do you reverse diabetes?
There are some new studies on reversing diabetes.
One of the studies shows that even a very small decrease in liver fat and especially pancreas that can restore normal beta cell function.
You can also reduce internal inflammation.
And you can reduce free fatty acid release that causes insulin resistance.
In fact, our bodies can burn either sugar or fat.
It’s more efficient to burn sugar for energy.
But a diabetic has impaired sugar metabolism.
There are many supplements and nutritional approaches that can reverse this inability to burn sugar.
By correcting this metabolic problem that diabetics have, they can reverse their diabetes.
And they will eventually lower blood sugar and restore healthy metabolism.
Citations
An update on the pathogenesis of type 2 diabetes mellitus
http://hamdanjournal.org/journal/index.php?journal=HAMDAN&page=article&op=view&path%5B%5D=167&path%5B%5D=283
https://www.researchgate.net/profile/Robert_Andrews2/publication/13089400_Andrews_RC_Walker_BR_Glucocorticoids_and_insulin_resistance_old_hormones_new_targets/links/568a4ec908ae051f9afa3fd6.pdf
Click for more information on Diabetes Mellitus, for information on Diet & Exercise, or for more on Diabetes.
