
So weird…but it works…
—-Important Message From Our Sponsor—-
Here’s proof of what really turns a woman on…

My friend has been doing a LOT of research on this kind of data lately…
And if you want to get your hands on the good stuff…
I mean like the kind of statistics that can literally increase your chances of getting laid – exponentially – I’m about to let you in on a HUGE secret…
But I’m warning you…
This is some real Big Brother type stuff.
The government is even involved.
Watch this where I explain everything — and show you the proof of what really turns a woman on…
———-
Take this — and you’ll look 12 years younger
How old you look has mostly to do with your skin. Aging skin looks old. Youthful skin makes you look young.
And now in today’s newsletter I unravel what makes youthful skin — no matter your chronological age.
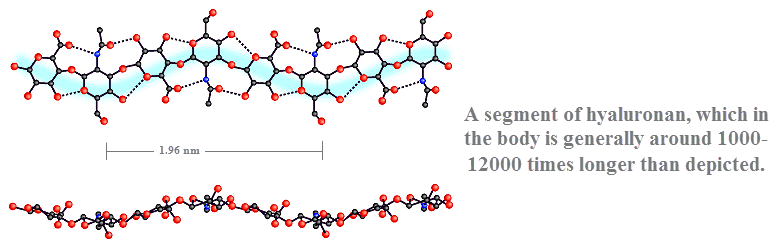
The biggest change that happens during skin aging is the reduction of hyaluronan.
Hyaluronan is a large molecular weight polymer composed of N‑acetylglucosamine and glucuronate in alternating sequence.
It has a unique capacity to absorb and retain water.
For this reason, hyaluronan (HYA) is responsible for contributing the most towards skin volume.
The progressive loss that accompanies aging supports this view.
The reduction of skin volume is the fundamental cause of wrinkles, which are (of course) associated with advancing age.
We have HYA throughout our body.
But especially in the skin, synovial fluid, and penis – where it might even contribute to “rockiness”.
From a 1995 study:
“The very high hyaluronan (HYA) content in the penis has not, to our knowledge, been reported previously. Considering the profound viscoelasticity of the HYA molecule, this may be of importance in the structural integrity and functioning of the connective tissues… It could well be involved in the physiology of erection.”
Knowing about the molecular changes that accompany aging skin is a step in the right direction… It could perhaps even prevent or reverse these changes.
Fortunately for us, science already knows about a few things that affect skin HYA balance…
Topical retinol, N‑acetylglucosamine, ascorbyl palmitate, and PPARα agonists increase HYA.
And cortisol has been shown to decrease HYA.
In fact, this reduction of HYA underlies the tendency of glucocorticoids to cause skin thinning – a classic side effect of topical hydrocortisone.
Cortisol is one of the few hormones that often increases with age.
And that may be a consequence of the decreased melatonin that also occurs with age.
Melatonin suppresses the release of corticotropin, the master regulator of adrenal cortisol synthesis.
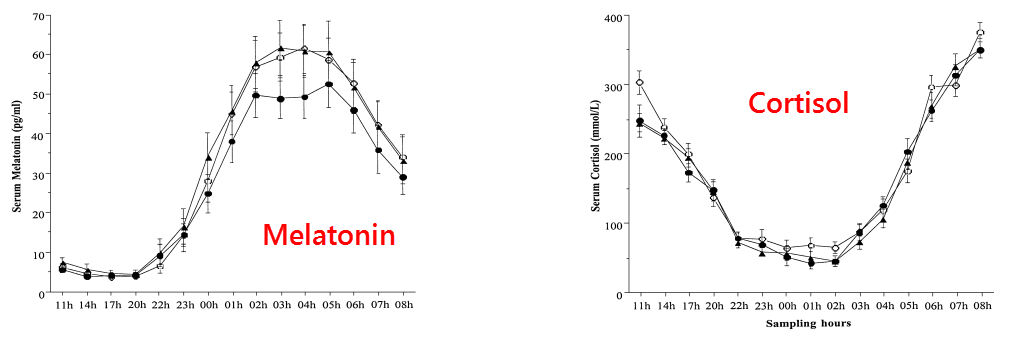
This is why corticosteroids also have a strong circadian rhythm that exactly mirrors that of melatonin:
So, along with the aforementioned substances that stimulate HYA synthesis (or inhibit its breakdown), anti‑cortisol drugs could be added to the list.
It’s intuitive why cortisol, a glucocorticoid, should do this – since HYA can be converted into fructose‑6‑phosphate and then metabolized.
This is the classic function of glucocorticoids – to liberate sugars during stress.
Although this is commonly thought to primarily occur through glycogen breakdown in the muscle and liver, there’s also evidence that HYA of the skin is a substrate.
For example, injection of cortisol significantly upregulates the enzyme hyaluronidase (HYAL).
HYAL degrades HYA in the livers and kidneys of rodents.
This could be seen as an evolutionary method to liberate glucose during stress…
Or also as a plasma expander during sodium deficiency.
Since cortisol activates both glucocorticoid receptors and mineralocorticoid receptors, either explanation could make sense.
But more modern data shows that glucocorticoids act to reduce HYA through downregulating an enzyme that makes it, hyaluronan synthase −2 (HAS‑2).
This has been shown to occur with many glucocorticoids including mifepristone, dexamethasone, betamethasone, mometasone, and clobetasol.
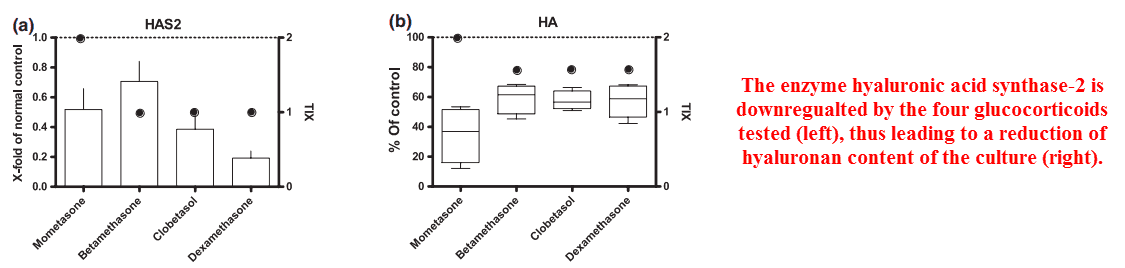
A significant reduction of HYA synthesis has also been shown with cortisol, yet the specific enzyme responsible wasn’t explicitly determined.
Since cortisol is a glucocorticoid that increases with age, it could be the prime suspect for age‑dependent reductions in skin volume.
It most certainly does this in part by downregulating HAS‑2, but perhaps also by increasing HYAL.
So it should be no wonder that compound K, a natural 11β‑HSD1 inhibitor (11β-hydroxysteroid dehydrogenase type 1inhibitor), has been shown to increase skin volume through HAS‑2:

Compound K is the main metabolite of ginsenoside Rb1 – a compound found in panax ginseng.
And good evidence suggests that it’s a potent 11β‑HSD1 inhibitor.
11β‑HSD1 transforms inactive cortisone into active cortisol.
So the inhibition of this enzyme is probably responsible for the anti‑stress, anti‑aging, and anti‑diabetic actions of panax ginseng.
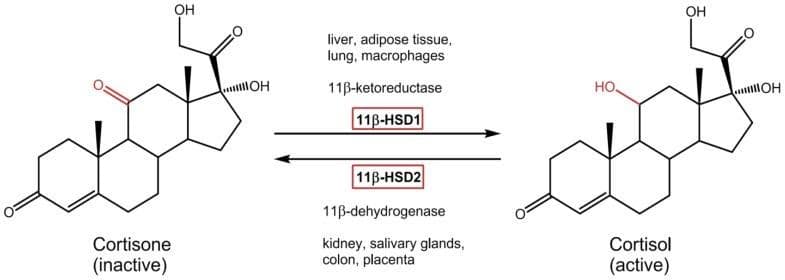
Based on previous reports, these researchers decided to investigate the effects of compound K on the skin more thoroughly.
This is what they did:
(1) Obtained panax ginseng root
(2) Extracted compound K from it
(3) Added it to human skin cells
(4) Applied microarrays to the mRNA extracted from those cells
The mRNA microarray is a common “shotgun technique” to visualize changes in expression by analyzing a multitude of genes simultaneously on one small “chip.”

They found that HAS‑2 was upregulated the most (4.8‑fold) out of more than 100 genes they looked for.
Then they further analyzed the largest changes in gene expression using PCR, a more accurate technique for determining changes in mRNA concentration.
From this, they showed that HAS‑2 normally isn’t even expressed in skin cells – but that it can be induced (dose dependent) by compound K at low concentrations.
Since HAS‑2 appears to be downregulated by cortisol, this is more indication that compound K is a potent 11β‑HSD1 inhibitor.

Predictably, this increase in HAS‑2 mRNA coincided with an increase in HYA content (2‑fold increase at the concentration of .1 μM) (3.3‑fold increase at 1 μM).
They also applied compound K to hairless mice and demonstrated an increase in skin HYA content and epidermal thickness.
“Consistent with the increased hyaluronan content, a pronounced increase in the epidermal thickness was observed in the compound K-treated murine skin.”
This could be why glycyrrhizin, another 11β‑HSD inhibitor, is often added to cosmetics.
Retinol is another common addition shown to increase HYA, and consistently so – shown for the first time over 30 years ago (King, 1984) and then at least four more times since.
Below is one of those studies:

These researchers were already well aware of the ability of retinol to induce HYA.
But they undertook this study to elucidate the details.
They also examined the effect of N‑acetylglucosamine (one of the building blocks of HYA), β‑carotene, and retinoic acid.
Not surprisingly, all four test compounds increased the synthesis of HYA.
The retinoids did so through gene induction and N‑acetylglucosamine acted as a substrate.
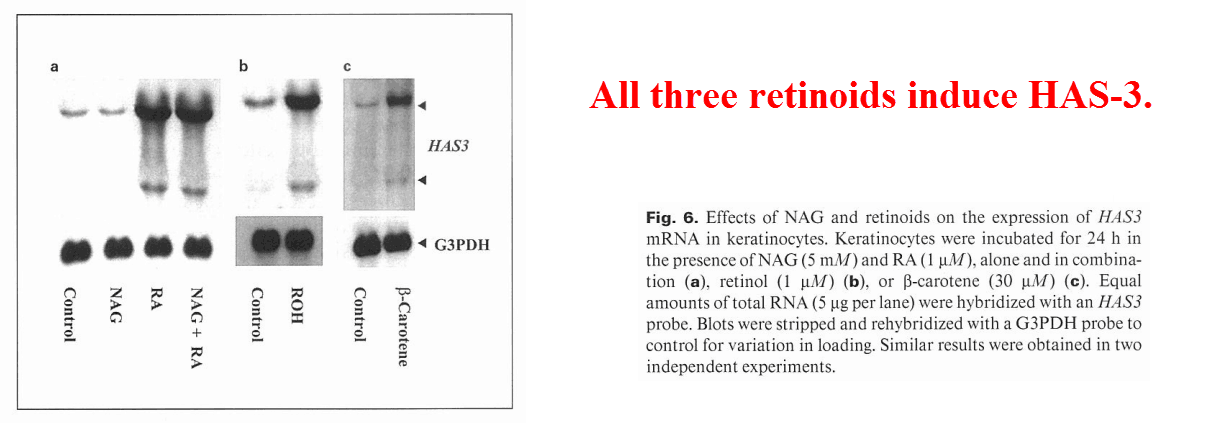
The retinoids didn’t influence the same enzyme that is repressed by cortisol, but an entirely different isoform called hyaluronan synthase‑3 (HAS-3).
This means that it should work synergistically with the 11β‑HSD1 inhibitors – since these increase the levels of HAS‑2, not HAS‑3.
Perhaps cooperative is a slightly more accurate word than synergistic…
And that’s because these two enzymes actually produce HYA polymers of slightly different chain lengths.
“HAS-1 and HAS-2 generate high molecular weight hyaluronan…while HAS-3 is involved in the production of lower molecular weight hyaluronan.”
There’s also indication that this effect is mediated through the retinoid X receptor (RXR) (Kim & Nam, 2006), meaning that phytanol should also work.
So reducing stress and consuming retinoids should help prevent wrinkles.
But there’s one more molecular class shown to do this…
Unlike the 11β‑HSD1 inhibitors and retinoids, HYAL inhibitors increase HYA not through promoting synthesis but by preventing breakdown.
Of this class of natural HYAL inhibitors, there is no other more useful than ascorbyl palmitate:

Ascorbyl palmitate is ideal.
And that is partially because it’s metabolized into vitamin C, necessary for collagen production.
But also because it’s one of the most potent HYAL inhibitors known.
These researchers found that ascorbyl palmitate had an IC50 of 4.2 μM on HYAL isolated from Streptococcus agalactiae – chosen for the research due to its commercial availability.
(IC50 is a measure of the potency of a substance in inhibiting a specific biochemical or biological function.)
And it had an IC50 of 56.5 μM on bovine testicular HYAL.
Also, a study published just this year provides convincing evidence that ascorbyl palmitate also inhibits HYAL‑2 in rodents (Zhu, 2019).
So when used topically or internally, these three drug classes – retinoids, 11β‑HSD1 inhibitors, and HYAL inhibitors – should help maintain skin volume with age.
Although we all will certainly age, there’s no reason why we can’t delay some of the effects.
“The hyaluronan content is reported to decline with age…which may contribute to wrinkle formation and the decrease in elasticity of the skin…” (Mayo, 2004)
“These results suggest that topical application of compound K may prevent and improve the cutaneous alterations caused by the decrease of the hyaluronan content in aged skin.” (Kim, 2004)
“The turnover rate measured by injected…hyaluronan is surprisingly rapid. The half-life of the injected polymer in skin and joints is only about 12 hrs…in the anterior chamber of the eye it is 1 to 1.5 hrs…although in the vitreous body [of the eye] it is 70 days.” (Laurent, 1992)
—-Important Message—-
73% more blood flow “down there”
Imagine the flood gates opening and blood rushing into your penile chambers…
…reaching every nook and cranny and making your member grow and get stiff and engorged.
It’s all thanks to simple, healthy supplements that clear out the penile chambers and increase blood flow…
It’s a simple supplement formula that any man can use to get big, strong, firm erections whenever they want…
And erections is better, more engorged, and lasting longer… you are able to perform at your best in bed, every single time…
Start experiencing 73% more penile blood flow today using this simple FREE formula
———-
