
[cmamad id=”23632″ align=”center” tabid=”display-desktop” mobid=”display-desktop” stg=””]
Do this — and you can show your friends and colleagues that you are smarter and remember more than they do. They will be so jealous…

—-Important Message—-
This natural white powder removes toxins that cause Alzheimer’s from the brain.
Research tells us that Alzheimer’s is caused by a toxic build-up of heavy metals in the brain.
These heavy metals are hiding in men’s shampoos and deodorants… They enter the bloodstream and travel to the brain.
And the more they build up there, the higher risk men have of developing memory problems or full-blown Alzheimer’s…
But don’t worry, because there’s a simple, almost miracle-like cure for getting rid of these toxins in the brain…
It’s a natural white powder that costs less than 89 cents at the grocery store.
And it’s been around so long, it’s basically a cure put here by God. That’s why Big Pharma doesn’t want you to know about it…
———-
Raise your choline and make your friends jealous of you…
To make your friends jealous, you just need to show them brainpower made possible from acetylcholine.
What is that?
Well, acetylcholine is one of the three primary neurotransmitters, along with dopamine and serotonin, and arguably the most important one.
Acetylcholine is the neurotransmitter we need to create the nerve potential required for movement and cognition.
Yet, unlike serotonin and dopamine, we have acetylcholine everywhere throughout the body.
The importance of acetylcholine in cognition is perhaps best demonstrated by acetylcholine mimetics (such as nicotine).
These increase reaction time, attention, and word recall.
The lowered amounts of acetylcholine (and its receptor) consistently found in Alzheimer’s disease also demonstrates its importance.
“Indeed, three compounds have received European approval for the treatment of the cognitive symptoms of Alzheimer’s disease – first tacrine and, more recently, donepezil and rivastigmine – all of which are cholinesterase inhibitors.”
The most common way – or the pharmaceutically preferred way – to increase acetylcholine has always been through using cholinesterase inhibitors…
This is the enzyme responsible for breaking it down.
Cholinesterase is an enzyme that degrades acetylcholine.
So any drug that significantly inhibits cholinesterase ultimately promotes higher acetylcholine concentrations through sparing it.
The beneficial effects of cholinesterase inhibitors in Alzheimer’s disease are attributed to their ability to increase acetylcholine…
And that neurotransmitter has long been noted for its prime role in cognition.
Yet science shows that there are many ways to increase acetylcholine…
Synthetic cholinesterase inhibitors are not the only way.
Expensive pharmaceuticals are preferentially used because more expensive and exclusive drugs translate to more money for doctors and pharmaceutical corporations.
So, yes, you can certainly spare acetylcholine by inhibiting cholinesterase, and improve cognition that way…
But you can also do it by ingesting its precursors and/or the proper B vitamins.
[cmamad id=”23633″ align=”center” tabid=”display-desktop” mobid=”display-desktop” stg=””]
Thiamine (B1), folate (B9), and cobalamin (B12) are the most important vitamins for acetylcholine synthesis.
We need vitamin B1 so we can transform pyruvate into carbon dioxide, acetate, and, ultimately, acetyl-coenzyme A.
This vitamin is the coenzyme we need for choline acetyltransferase, which marks the final step in acetylcholine synthesis.
Although not strictly a vitamin, alpha-lipoic acid is also important.
That’s because, along with thiamine, alpha-lipoic acid is also a coenzyme for pyruvate decarboxylase.
Alpha-lipoic acid physically transfers the acetyl group from the enzyme-bound thiamine molecule to acetyl-coenzyme A.
And then that diffuses away towards choline acetyltransferase and subsequent choline synthesis.
Moreover, alpha-lipoic acid is also a coenzyme for choline acetyltransferase.
“Neurons obtain choline from 2 sources: uptake from serum choline mainly derived from dietary intake and de novo synthesis.”
Vitamin B9 also acts to increase acetylcholine, at least in people who are deficient in it.
Folate (B9) is unique in that it can create completely new methyl groups via the amino acid L-serine, of which choline needs three.
Vitamin B12 has a central cobalt atom that binds methyl groups.
And then those are transferred to S-adenosylhomocysteine thus forming S-adenosylmethionine.
This cofactor is also freely diffusing and carries methyl groups that can be used for choline synthesis – most of which were initially created by folate.
Yet science shows that choline can more or less bypass vitamins B9 and B12 by obviating the need for its own synthesis.
Our bodies don’t need to create choline from scratch if we eat lots of it…
(Choline is in meat, poultry, fish, dairy products, eggs, cruciferous vegetables, and some beans.)
This is analogous to how cholesterol intake reduces the obligation for our bodies to make cholesterol.
Yet we still need these vitamins for other things, such as for DNA synthesis and lowering homocysteine (an amino acid in our blood that we get from eating red meat).
So I don’t want to give the impression that we don’t need folate, because we do…
At least for synthesizing three of the four DNA nucleotides.
“We propose that the availability of circulating choline constitutes an additional factor controlling the synthesis of brain acetylcholine.”
Choline’s ability to increase brain acetylcholine was demonstrated in the 1970s, showing us yet another way besides the aforementioned vitamins and drugs.

These scientists worked at MIT along with John Fernstrom.
Previously, they showed how other diet-derived factors are involved in neurotransmitter synthesis.
For instance, they determined a few years previously that a specific plasma tryptophan ratio (tryptophan over the sum of five competing amino acids) was essentially a direct indicator of brain serotonin synthesis in real time.
“Hence, precursor availability may influence the synthesis of brain acetylcholine in vivo, just as it controls the synthesis of brain serotonin and brain catecholamines.”
Brain dopamine is also under the control of tyrosine, and phenylalanine to a lesser extent.
Continuing along this line, these diet-neurotransmitter researchers provided us with the earliest demonstration of brain acetylcholine being created from choline.
Previously, there were failed attempts to do this. They failed because of improper handling techniques that allowed acetylcholine to degrade before analysis.
This particular study was the first to microwave the rats to death…
And that inactivated the enzyme cholinesterase and therefore preserved all brain acetylcholine until they could measure it:
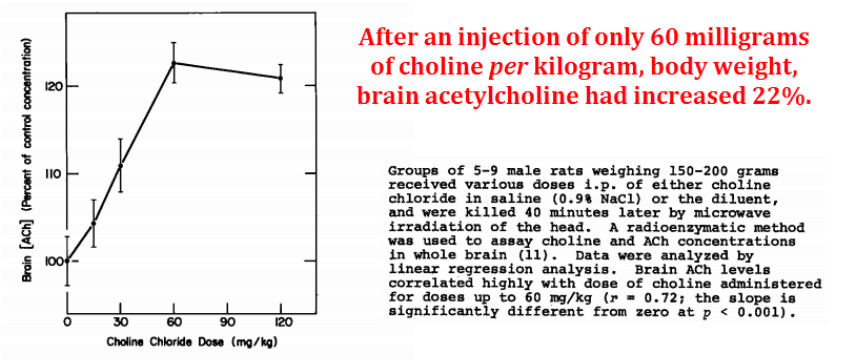
This was dose-dependent up to 60 mg/kg (at least in rats), after which it leveled off.
Since humans have a larger brain to body ratio, we might need a bit more than rodents to achieve the maximum effective dose.
Not many people would be willing to inject choline, especially if they could simply consume it instead.
Well, luckily for us, choline does work orally.
A follow-up study, published one year later in the journal Science, proved just that:

A year later, the MIT researchers used the same Sprague Dawley rat strain as in the previous study.
But this time they gave them choline in their drinking water, in three escalating doses, for eleven days.
They also used the same microwave method to kill them, thus preserving acetylcholine.
(Incidentally, this was actually just a modified Litton microwave, the same as what people cooked food with in the 1970s… Though in some parts of the world, rats might be considered as food.)
And these researchers got the expected result: Dietary choline definitely increased brain acetylcholine:
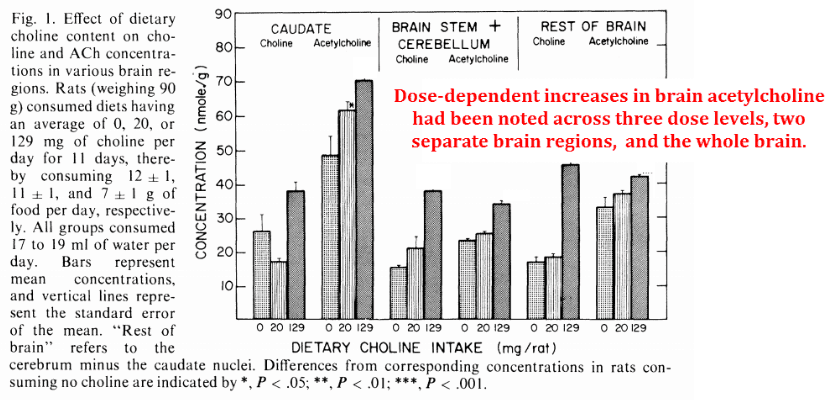
Moreover, these dose levels were in the range of what humans consume daily…
Eggs have the highest choline concentrations of any common food (exclusively in the yolk), followed by beef and fish.
And broccoli, kale, and Brussels sprouts aren’t far behind…
Cheese and peanuts also have decent amounts.
Betaine is a similar molecule and it is also found in many foods such as spinach, beets, wheat, and shellfish.
Although betaine doesn’t directly go towards acetylcholine synthesis, it does spare methyl groups thereby taking a burden off of folate.
“We show that physiological variations in choline content in the diet (that is, variations within the range that omnivorous animals or humans might consume from day to day) are associated with parallel changes in brain acetylcholine concentrations, especially within the caudate nucleus.”
Yet, the ideal would probably be to ensure you consume sufficient folate and vitamin B12 – at least for making acetylcholine yourself when you’re not eating the aforementioned foods.
And remember that ingesting choline does not make up for our need for thiamine and alpha-lipoic acid…
We need these two to make the acetyl groups.
These scientists also found a good correlation between serum choline and brain acetylcholine, suggesting that choline readily enters the brain.
This is what you’d expect, since choline is quite small and lipophilic (tending to combine with or dissolve in lipids or fats).
“A significant fraction of plasma and, therefore, brain choline is of dietary origin.”
So all the way up until the “enzyme saturation point” – after which additional choline would do nothing – brain acetylcholine is a direct function of serum choline concentration.
And that, in turn, is a direct function of dietary choline intake.
But there is one thing to point out about this study…
They probably gave these rats folic acid and not natural folates.
Folic acid is a low-activity synthetic form that converts primarily into an inactive metabolite, the (6S)-enantiomer, in the liver.
There is even reason to suppose that folic acid is an antifolate drug…
As such, it would inhibit crucial enzymes and receptors along with its inactive (6S)-metabolite.
The published study didn’t include information that would allow you to infer the rats’ vitamin B12 status…
But since this is produced by enteral bacteria, we could assume that vitamin B12 deficiency has as much to do with antibiotics, probiotics, and yeast overgrowth as it does with dietary intake.
As convincing as these two studies are, perhaps even enough to “close the book” on this, there was another confirmation just one year later.
This study was of a somewhat different sort:

These researchers used the same Sprague Dawley rat strain as the two previous studies.
They also used the same drinking water route to get choline into them…
But this one measured acetylcholine more indirectly.
Instead, they measured the brain concentrations of the acetylcholine receptor, which they determined by the most accurate means possible:
“The resulting supernatants of brain and muscle were assayed for acetylcholine receptors using 1251-alpha-bungarotoxin, which binds to these receptors with unparalleled affinity and specificity.”
Some snakes (i.e. the many-banded krait) produce this toxin – it’s why their bites are paralytic…
The toxin inhibits the acetylcholine receptors of the snake’s prey, making the victim unable to move.
These rats drank choline dissolved in their water (15 gms/L) for three weeks.
At that point, the researchers found significant increases in brain acetylcholine receptors.
This is the same receptor, mind you, that is reduced in the demented brain.
This implies that dietary choline – as with vitamins B1, B9, and B12 – could be a good way to help ward off dementia or to increase general brainpower.
“Significant differences in the density of acetylcholine receptors were observed in the cerebral hemispheres (48% increase in the high choline group) and forebrain (43% increase)…a slight but significant increase was found in the brain stem.”
We also need acetylcholine for muscle contraction, which makes it an anabolic neurotransmitter.
A similar study showed a 30-35% decrease in brain acetylcholine using only 1/10 of the dose (1.5 gm/L).
It is reasonable to believe that this does work for humans too.
A small clinical trial using people with Huntington’s disease showed a definite improvement (Davis, 1976).
And epidemiological studies have correlated choline intake with verbal memory and learning (Poly, 2011).
The 1976 study by Kenneth Davis was particularly interesting…
They showed the effects of gram-sized doses lasting longer than 48 hours, which is the plasma clearance time.
This suggests that excess choline was stored as phosphatidylcholine on brain lipid membranes.
And maybe that provides a ready-made source that we can draw on during times of low dietary intake.
“Phospholipid-bound choline may constitute a long-acting pool of free choline in brain through its hydrolysis, even after exogenous choline is discontinued.”
And, although only six out of the eight patients in that study improved, they were the same six who also responded to the cholinesterase inhibitor physostigmine.
So, despite it not working in two of the eight patients, this fact strongly implies that acetylcholine was increased in the adult human nervous system.
In other words, since physostigmine didn’t work for the same two patients, their disorder wasn’t due to a lack of acetylcholine anyway.
No cholinergic drug would have helped those cases…
Not even acetylcholine itself would have worked.
Those cases probably had more to do with dopamine.
So all the available evidence indicates that acetylcholine improves brain function.
And it indicates that affordable vitamins, cofactors, and precursors (the ones you’d want anyway) are a very effective way to increase it.
Taking all of them could even be more reliable than the three pharmaceutical FDA-approved cholinesterase inhibitors: tacrine, donepezil, and rivastigmine.
Alpha-lipoic acid and thiamine (B1) work together to synthesize the acetyl half of acetylcholine. And folate (B9) and cobalamin (B12) help to synthesize the choline part.
Yet it has been proven that the dietary intake of two of those vitamins can be made redundant by taking choline directly, at least for this purpose.
“Because the range of choline consumption used in the two groups was within the range of variation that could occur in the human diet, we suggest that alteration in diet can alter brain function… The possibility of altering such behavior by dietary manipulation has profound implications.”
Yet choline isn’t 100% innocuous… It has been shown to increase platelet aggregation by about 30% at 450 mg/day.
This effect was been lowered by aspirin, which highlights the role that thromboxane (A2) plays in thrombosis.
So perhaps a lower amount of around 300 mg/day of choline – a commonly sold dose – should be used for acetylcholine synthesis, as needed.
Alternatively, a person could rely a bit more on the B-vitamin route for brain choline synthesis and perhaps a bit less on supplemental choline.
Either way, you will be 10 or 20 IQ points smarter, and you’ll recall movies, and events from the past, and stuff you read — that will make your friends’ and colleagues envious of you…
—-Important Message—-
I’ve never had better erections in my life — my poor girlfriend was sore but smiling but sore the next day…
I used to struggle with getting erections.
And I was always wondering if it was going to rise to the occasion.
But now, it’s completely different.
I discovered a simple activity that gives a man erections like he had when he was 20.
So once you go to bed with your wife or girlfriend, you and she will be quite amazed.

Then it will become second nature and you’ll wonder why it was so difficult for you before.
So why does this solo activity work so well?
It works by reversing ALL THREE of the most common causes of ED.
And it restores great sensation…while letting you last 30 minutes or longer…
It works a little like weight-lifting.
Little by little, every time you do it, this activity strengthens your penis and increases sensation.
So the next time you’re with a woman, you can get great, powerful erections that last 30 minutes or more.

———-

- Cohen, E. "Brain acetylcholine: increase after systematic choline administration." Life sciences (1975) http://sciencedirect.com/science/article/pii/0024320575901940
- Cohen, E. "Brain acetylcholine: control by dietary choline." Science (1976) http://sciencedirect.com/science/article/pii/0024320575901940
- Morley, B. "Effects of dietary choline on nicotinic acetylcholine receptors in brain." Nature (1977) http://nature.com/articles/266848a0
- Nagler, A. "Tissue levels of acetylcholine and acetyl cholinesterase in weanling rats subjected to acute choline deficiency." The Journal of nutrition (1968) http://academic.oup.com/jn/article-abstract/94/1/13/4778074
- Choline — Health Professional Fact Sheet https://ods.od.nih.gov/factsheets/Choline-HealthProfessional/
- Choline | Linus Pauling Institute | Oregon State University https://lpi.oregonstate.edu/mic/other-nutrients/choline
